
Bladder prolapse is a common issue that affects women across the world. Also known as cystocele, this problem occurs when the anterior vaginal wall is debilitated and stretched, causing the bladder to bulge in the vagina. The bladder drops from the pelvic cavity and sticks through the anterior vaginal wall.
This can cause a series of uncomfortable symptoms such as pain, discomfort and problems urinating, even urinary or fecal incontinence. Although bladder incontinence is not dangerous on itself it can be weakening and it has a significant impact on someone’s quality of life.
According to the latest studies and demographic samples, the prevalence of any degree of prolapse is estimated to be 30,8% in women aged 20-59 and that based on the a scientific publication of the ELSEVIER magazine each year an estimated 200.000 surgical interventions are carried out due to a prolapsed female pelvic organ (FPO), making it one of the most common procedures.
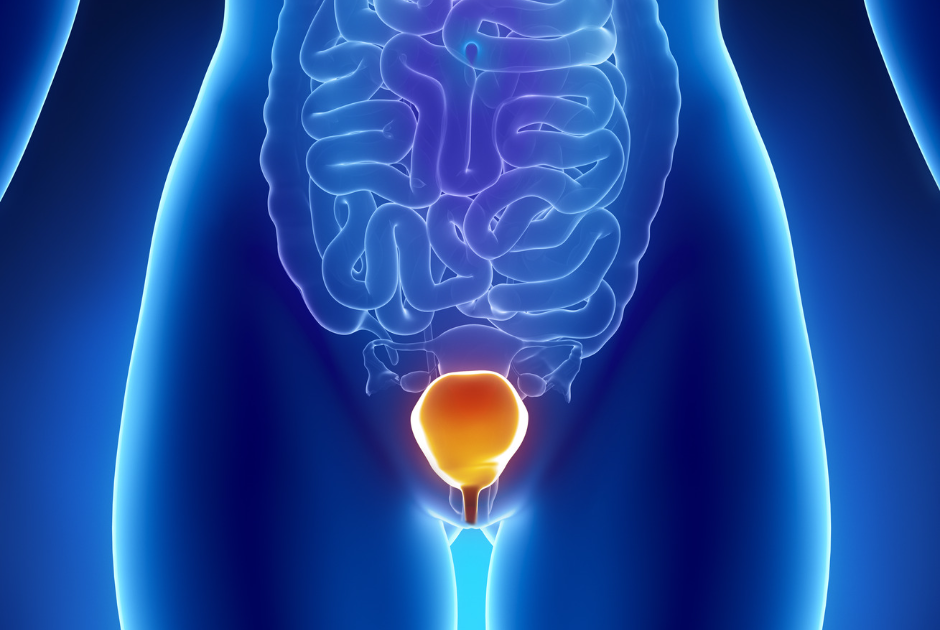
Luckily, physiotherapy can effectively treat and prevent a bladder prolapse.
What are the causes and symptoms of bladder prolapse?
The main causes of bladder prolapse are the absence of adequate support from the ligamentous system that holds the bladder in place, combined with the lack of firmness of the vaginal wall tissue. This can be caused by genetic and hormonal factors, as well as age. This is why a bladder prolapse tends to appear after childbirth or during menopause. It is also more present in more women who practice impact sports such as running and jumping or smokers with a chronic cough.
With regards to the symptoms of bladder prolapse, in mild cases it ‘s possible for the patient not to show any signs or symptoms. Possible symptoms include:
- Feeling of heaviness or pressure on the pelvis and the vagina.
- A visible or tactile bump in the vaginal tissue.
- Increase of the pelvic pressure when overexerting, coughing, squatting or getting up.
- Problems when urinating, even difficulty to start a urine stream, the feeling of not being able to completely empty the bladder when urinating, the need to frequently urinate or urine loss (urinary incontinence).
How to treat bladder prolapse
As with any type of prolapse, there are different grades of cystocele.
From a grade I, where the prolapse is not visible from the outside and can only be detected through vaginal exploration up to a grade IV, where the bladder almost completely sticks out of the vagina, requiring surgical intervention.
For the treatment of grade I and II bladder prolapses, it is recommended to train the pelvic floor with the help of hypopressive and Kegel exercises.
In case of a grade II or III, when a woman experiences discomfort carrying out daily activities, she may be requested to use a pessary to soothe the symptoms.
Grade III or IV are the most severe and the only solution is a surgical intervention to reposition the bladder stitching it back into its original position or adding a surgical mesh to avoid it from dropping again.

It certainly is true that most women consulting physiotherapists on the matter, mention a feeling of ‘heaviness’ inside the vagina. Sometimes they don’t feel it, but the physiotherapist will detect it during the intracavitary exploration. Many of them have spoken with their doctor and they’ve only been told about the surgical option or, at the most, they have been recommended visiting a physiotherapist for specific exercises.
Is there anything else we can do to treat bladder prolapse, apart from exercises?
Thanks to Capenergy’s Tecar Evolution technology and its C500 Urogyne device, designed specifically for the treatment of gynecological pathologies, non-invasive treatments can be carried out that largely improve the symptoms of bladder prolapse, thus avoiding surgery and its side effects.
During prolapse rehab, apart from increasing the pelvic floor muscle tone and strength, that support all the pelvic organs from below, it is important to increase the trophism of the ligamentous and fascial system that support the organ.
This is where manual techniques and exercises fall short.
We need to regenerate the collagen that has lost its properties and generate new collagen and elastin fibers to restore the tissue tension and firmness. With CAPENERGY’s technology we can do this in a non-invasive, efficient, painless and secure way.
Capenergy’s second generation tecar therapy device is on of the fastest and most efficient tools for tissue vascularization, increasing trophism and muscle tone. It furthermore allows creating new collagen type I, type III and elastin fibers, thanks to the temperature increase generated by the Capenergy’s patented intracavitary probe, equipped with 2 temperature sensors that assure the patient’s safety at all times.
Other advantage of the CAPENERGY C500 intracavitary probe, is its anatomic shape that facilitates access to the vagina and carry out a series of leverage movements and mechanical mobilizations with a completely safe 360º emission of radiofrequency. This generates a vascularization of the area and a hypothermic effect, leading to the generation of new collagen and elastin fibers that strengthen the vaginal walls and muscles.
Capenergy’s technology, with its correspondent medical CE and recognized sanitary indications differs from other tecar therapy devices as it offers 4 specific accessories for the treatment of urogynaecological pathologies, both male and female.
It’s important to highligh the intracavitary MJS probe, a capacitive electrode with a specific anatomic finger shape.
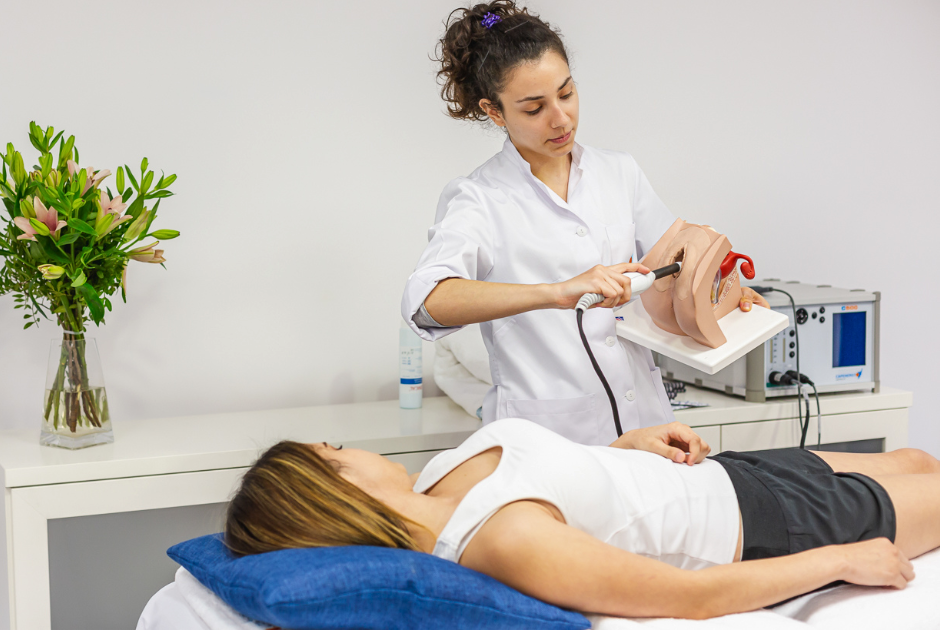
Unlike other intracavitary RF probes, the MJS probe is equipped with a temperature sensor, so it can work at temperatures of up to 45ºC without any discomfort or risk. The patient only perceives a pleasant warmth during the treatment and a feeling of lightness in the abdominal and pelvic area after the session has come to an end.
This treatment furthermore has other more general benefits:
- Even though we are talking about a bladder prolapse, the treatment will concentrate mostly on the fascial endopelvic system as it acts globally. This way we can prevent future prolapses of other pelvic organs, such as the urethra, the uterus and the rectum.
- During the treatment session with the MJS probe, the physiotherapist can have the patient performing hypopressive or Kegel exercises at the same time. This will help the patient carry out the exercises more efficiently, as the increase of trophism will make the muscles contract more easily, apart from generating a more subjective perception of the contraction.
- Improvement of the vaginal lubrication, thanks to the trophism increase of the vaginal mucosa, decrease of the vaginal dryness and increase of the sexual response. Mejora de la oclusión vaginal y la sensibilidad durante las relaciones.
- On an aesthetic level, the visual aspect of the vulva is also improved.
The application options of Capenergy’s C500 Urogyne or not only limited to intravaginal or intraanal treatments. You can increase its functions by means of an UPGRADE, equipping the device with extracavitary accessories that allow working on an external level with manual and / or an automatic capacitive plate of 200cm2, also equipped with a temperature sensor.
CAPENERGY’s C500 is definitely useful not only for the treatment of bladder prolapses and an efficient alternative to surgery but also for the treatment of other common urogynaecological pathologies such as: fibrosis, endometriosis, dysmenorrhea, rectocele, coccygodynia, vaginisme, c-section, episiotomy and chronic pelvic pain in general.
Would you like to know more about Capenergy’s tecar therapy and how it can help you multiply your clinic’s profits? Request your free demo.