Urinary incontinence after radical prostatectomy is a physically and emotionally demanding challenge.
Recovering from a radical prostatectomy is a physically and emotionally demanding process. When urinary incontinence—involuntary urine leakage that can develop after surgery is added to that process, the patient’s quality of life is significantly compromised. However, a non-invasive, safe, and clinically proven therapeutic option is now available.
In this article, we explore how Capenergy’s second-generation radiofrequency is proving to be an innovative and effective solution for the treatment of post-prostatectomy urinary incontinence (PPUI). We explain how it works, what backs its efficacy, and the benefits it can provide both your clinic and your patients from the very first sessions.
What is urinary incontinence after radical prostatectomy?
Radical prostatectomy is the most effective surgical treatment for prostate cancer, but like any major surgery, it can leave functional sequelae. Urinary incontinence is one of the most frequent and difficult to manage. It occurs mainly due to damage to the urethral sphincter during surgery, unabling the patient to control regular urine production.
According to the International Continence Society, urinary incontinence is defined as any involuntary loss of urine. In the case of PPUI, its prevalence varies between 2.5% and 90% depending on the time elapsed since surgery and the evaluation criteria used, and its impact on the patient’s quality of life is profound, affecting social life as well as emotional and sexual well-being.
Key risk factors for post-prostatectomy urinary incontinence include patient age, surgical technique, pelvic floor condition, time since surgery and pre-existing comorbidities.
Most common symptoms of PPUI
Although each patient’s experience is different, the most common symptoms reported by men with PPUI include:
- Urine leakage with effort: coughing, sneezing, getting up or physical activity.
- Urinary urgency: sudden, compelling urge to urinate that cannot always be controlled.
- Increased daytime and nighttime urinary frequency (nocturia).
- Need to regularly use pads or absorbent products.
- Emotional impact: embarrassment, social isolation and reduced daily activity.
Causes and factors influencing PPUI
The main cause of PPUI is damage to the external urethral sphincter during surgical resection. However, there are factors that can influence both its onset and severity:
- Patient age: patients of older age are at increased risk of persistent incontinence.
- Type of surgical technique used: robotic, open or laparoscopic surgery.
- Preoperative pelvic floor status.
- Time since surgery: most patients improve in the first months, but a significant percentage persists with symptoms at one year.
- Presence of previous urinary incontinence or comorbidities such as diabetes or hypertension.

When multiple risk factors are present, a personalized treatment plan is essential. Capenergy radiofrequency offers a clinically supported option to accelerate recovery.
When these factors combine, the recovery of continence can be slow and frustrating. This is where Capenergy’s radiofrequency offers a solid therapeutic alternative, backed by scientific evidence published in internationally recognized medical journals.
Traditional treatments for post-prostatectomy urinary incontinence
For years, the management of PPUI has focused primarily on two approaches: conservative pelvic floor rehabilitation and, in more severe or persistent cases, surgical intervention. While both have their place in clinical management, they present significant limitations.
Most common conventional approaches
Pelvic floor muscle training (PFMT):This is the first-line treatment for PPUI. Studies show it can achieve continence rates of 90% at 7 months after surgery. However, the process is slow, requires high patient adherence and incontinence may persist despite treatment.
Biofeedback and electrical stimulation:Complementary techniques to PFMT that help the patient become aware of the perineal musculature and improve neuromuscular control. They require multiple sessions and results vary.
Pharmacological treatment:Used in cases of associated urgency incontinence, with limited results and possible systemic side effects.
Surgery:Reserved for the most severe and persistent cases: artificial urinary sphincter or male suburethral sling. These are effective but invasive options with their own surgical and postoperative risks.
Many patients seek alternatives that accelerate their recovery, are less invasive and can complement or advance the rehabilitation process. This is where Capenergy’s radiofrequency technology represents a real turning point.
How can Capenergy help patients with PPUI?
Capenergy’s second-generation radiofrequency represents a significant advance in the conservative management of post-prostatectomy urinary incontinence. Its capacitive and resistive electric transfer (TECAR) technology acts directly on deep tissues, stimulating the body’s natural regeneration mechanisms.
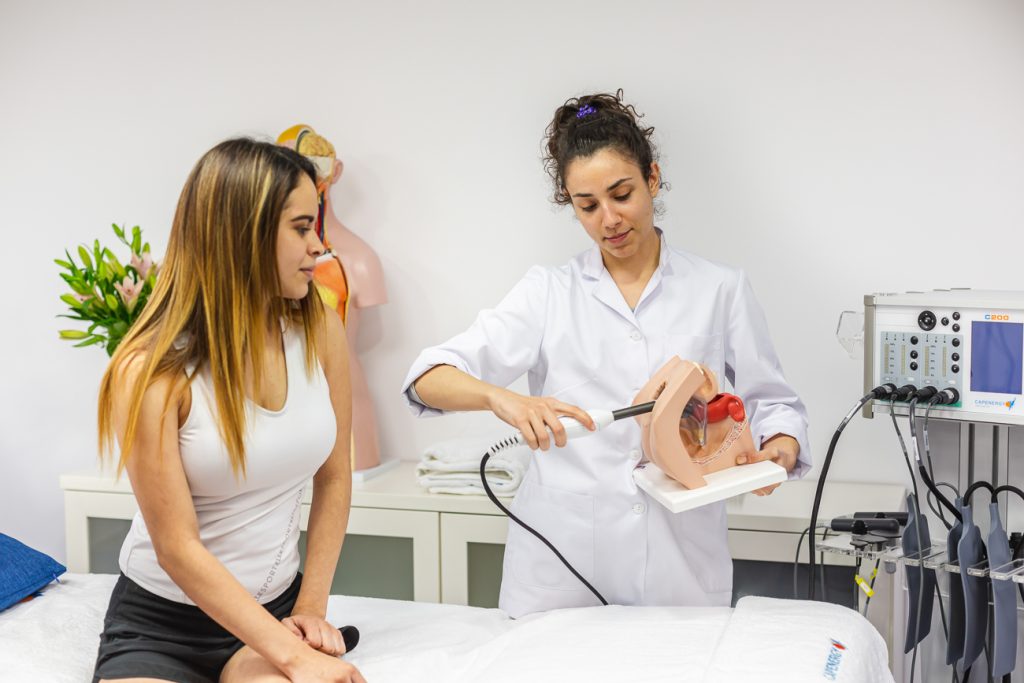
Capenergy radiofrequency with intracavitary electrode for non-invasive treatment of post-prostatectomy urinary incontinence.
The treatment is applied using a non-ablative endoanal electrode at a controlled temperature of 41°C, which stimulates collagen production (neocollagenogenesis) and improves vascularization of the periurethral tissue and male pelvic floor. This profound endothermal effect promotes the recovery of sphincter function without the need for any invasive intervention.
The results are supported by clinical studies published in top-tier scientific journals, such as Lasers in Medical Science (Springer, 2019), and presented at the American Urological Association Annual Congress (The Journal of Urology, 2018) and the International Continence Society (ICS) congress.
Demonstrated clinical results
- 70% reduction in urinary leakage: Pad Test dropped from 6.5 g to 2.0 g (p<0.01).
- 9 out of 10 patients experienced significant improvement in urinary leakage.
- 3 patients achieved complete resolution of incontinence.
- Significant reduction in irritative lower urinary tract symptoms (ICIQ-OAB, p=0.01).
- No change in post-void residual volume: safe technique with no relevant adverse effects.
- High patient satisfaction: 6 satisfied, 2 very satisfied, only 2 unchanged.
Benefits of Capenergy treatment
- Rapid and objective reduction of urinary leakage from the first sessions.
- Stimulation of neocollagenogenesis and improvement of periurethral vascularization.
- Non-invasive technique, no needles or aggressive maneuvers.
- Fully compatible with pelvic floor training and other conservative therapies.
- Can advance or complement post-surgical rehabilitation.
- Brief and well-tolerated protocol: 5 sessions of 2 minutes of effective application.
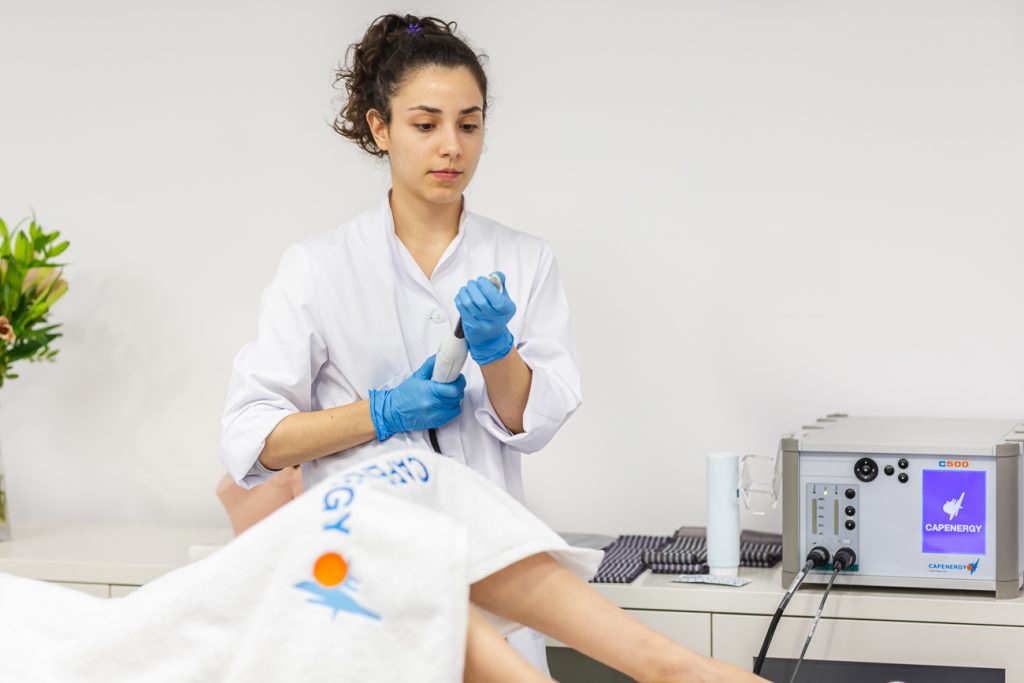
Capenergy: advanced technology for male pelvic floor rehabilitation. Differentiate your clinic with clinically supported solutions.
Do you want to incorporate this technology into your clinic?
Post-prostatectomy urinary incontinence is one of the most demanding therapeutic challenges in urology and pelvic floor physiotherapy. It requires an empathetic, respectful approach with maximum clinical rigor. With Capenergy radiofrequency, you can offer your patients a non-invasive alternative, backed by scientific evidence, that complements or enhances conventional treatments.
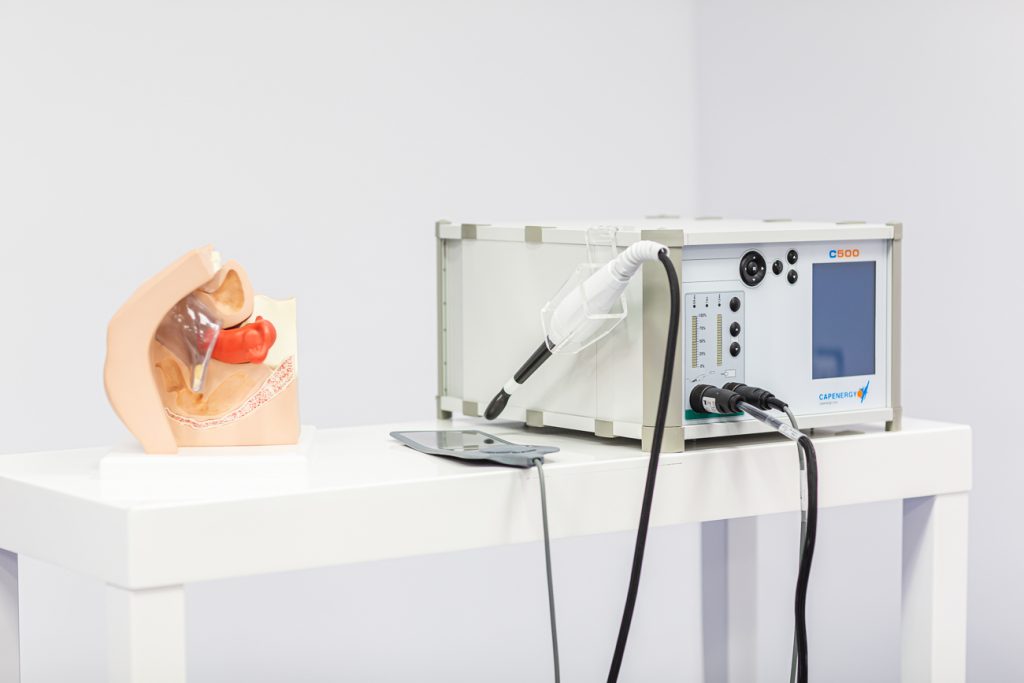
The Capenergy C500 with intracavitary electrode: second-generation TECAR radiofrequency for advanced pelvic floor rehabilitation.
Our Tecar Evolution family devices include the urogynecological module with intracavitary electrode, specifically designed for pelvic floor applications in both men and women. Its temperature control system guarantees therapeutic precision in every session, and the option for automatic or manual application allows the protocol to be adapted to each clinical case.
Benefits for your clinical practice
- Objective, measurable results from the first sessions.
- Safe, well-tolerated treatment with no known side effects.
- Scientific evidence published in urology journals and presented at international congresses.
- High patient loyalty for a condition with high emotional impact.
- Compatible with pelvic floor physiotherapy, biofeedback and electrical stimulation.
- Urogynecological module available for Tecar Evolution C100 devices and above.
Differentiate your clinic with the most advanced technology for male pelvic floor rehabilitation. With Capenergy, you can offer your PPUI patients a clinically proven, safe and non-invasive solution that shortens recovery times and significantly improves their quality of life. Contact us and request a free demonstration.
Frequently asked questions about PPUI treatment with Capenergy
- Is Capenergy radiofrequency treatment for PPUI painful? Most patients tolerate it well. In some cases, inserting the endoanal electrode may cause mild initial discomfort that disappears during application. The predominant sensation is of gentle, relaxing warmth in the pelvic area.
- How many sessions are needed to see results? In the reference clinical study, significant improvements were obtained after 5 sessions. Most patients report progressive improvements from the first applications.
- Can it be combined with pelvic floor training? Yes, and it is in fact recommended. Capenergy radiofrequency acts on connective tissue and vascularization, while PFMT works on the active musculature. Combining both strategies enhances results.
- From what point after surgery can treatment begin? The study excluded patients with fewer than 45 postoperative days. In general, it is recommended to start treatment once the acute phase of surgical recovery has passed and the patient is under medical supervision.
- Are the benefits maintained long-term?Study results show sustained improvements after the 5 sessions of the protocol. As with other conservative techniques, a maintenance plan is recommended to consolidate results and prevent recurrence.